TMS Therapy vs EMDR: Understanding Your Options Beyond Medication
TMS therapy vs EMDR: Learn how each treatment works, what conditions they target, and how to decide which option fits your mental health needs.
Choosing between two well-known mental health treatments can feel more complicated than it should. The conversation around TMS therapy vs EMDR has grown in recent years, but awareness does not automatically mean clarity. These treatments are built on entirely different models. Both are evidence-based. Both serve specific purposes. But they are not designed to do the same thing.
To make sense of the choice, it helps to understand how each treatment works, what symptoms they target most effectively, and how clinicians determine the right fit.
For those weighing TMS therapy vs EMDR, a personalized evaluation can clarify which approach aligns with your symptoms and goals. Learn more about available treatment options at charakcenter.com.
Two Treatments, Two Different Models
Before comparing outcomes, it helps to understand what each treatment actually is. TMS therapy and EMDR are built on very different models of care.
What Is TMS Therapy?
%20Therapy%20Equipment%20in%20Clinical%20Setting.png)
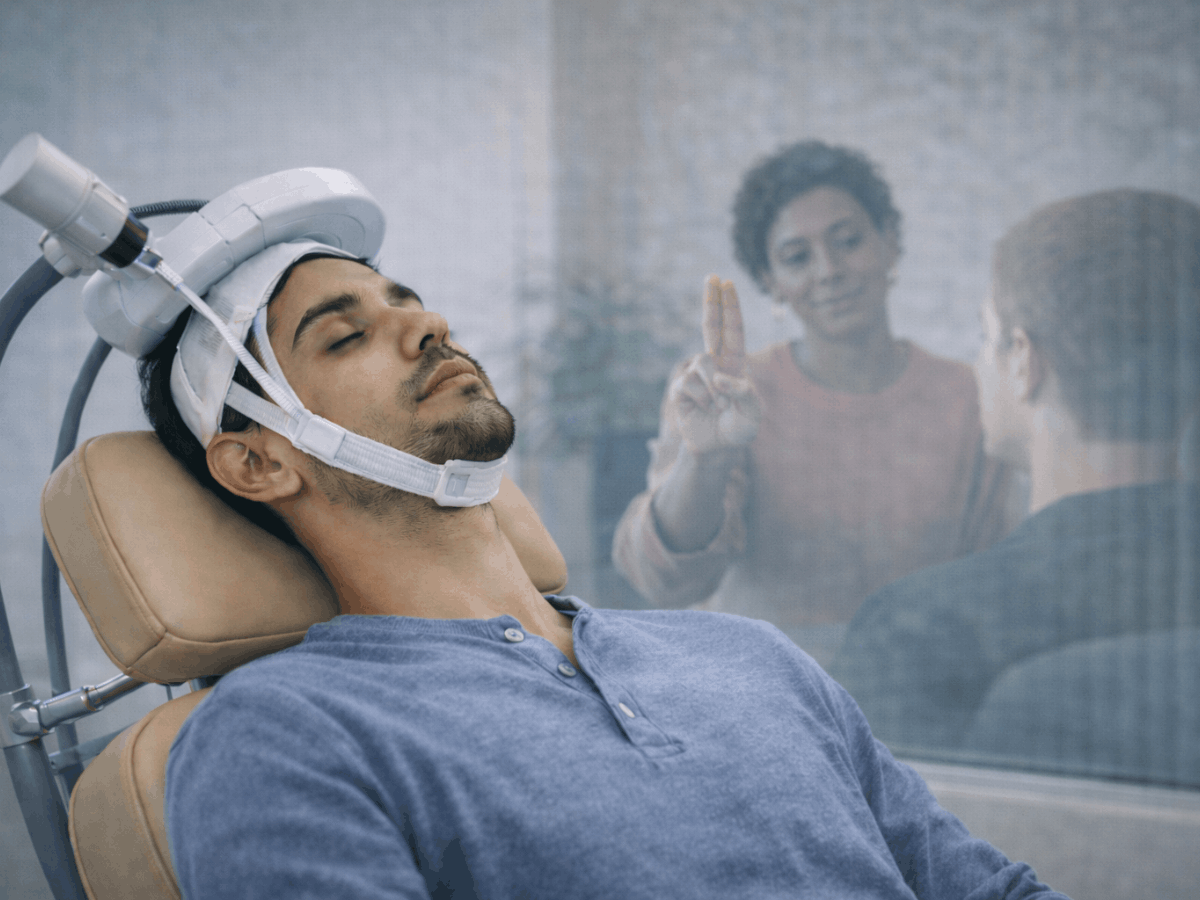
TMS therapy, or transcranial magnetic stimulation, is a noninvasive brain stimulation approach that does not involve surgery or anesthesia. Clinical studies show that among individuals with treatment-resistant depression, approximately 50 to 60 percent experience a meaningful reduction in symptoms, and about 30 to 35 percent achieve full remission following a full course of treatment.
During a session, a specialized device delivers focused magnetic pulses through a coil placed on the scalp. These pulses stimulate nerve cells in targeted areas of the brain involved in mood regulation. In individuals with major depressive disorder, certain regions of the brain may show reduced activity. TMS is designed to increase activity in those circuits and help restore more balanced brain function.
Common uses include:
- Major depressive disorder MDD, particularly when standard treatments have not been sufficient
- Obsessive compulsive disorder (FDA-cleared protocols)
- Certain anxiety symptoms, depending on clinical context
- Ongoing research in areas such as smoking cessation
TMS sessions are conducted in a clinical setting, and most patients return to normal activities immediately afterward.
What Is EMDR?

Eye Movement Desensitization and Reprocessing (EMDR) is a structured psychotherapeutic approach that helps individuals reprocess distressing memories so they carry less emotional intensity over time. Research shows it can be highly effective for post-traumatic stress disorder, with studies reporting that approximately 84% to 100% of individuals with single-incident trauma no longer met PTSD criteria after three to six 90-minute sessions.
It focuses on helping individuals process distressing or traumatic memories that may continue to influence current symptoms. During EMDR sessions, the therapist guides the patient through recall of specific memories while using bilateral stimulation. This can include guided eye movements, tapping, or auditory tones.
The goal is to help the brain reprocess stored traumatic experiences in a way that reduces their emotional intensity.
Common uses include:
- Post-traumatic stress disorder (PTSD)
- Trauma-linked depression
- Certain anxiety disorders
Unlike TMS, EMDR is talk therapy–based and centers on cognitive and emotional processing rather than direct brain stimulation. Its effectiveness in treating trauma-related conditions has been supported through ongoing clinical research that examines evidence-based approaches to mental health care.
How Each Treatment Is Tolerated
Nearly half of individuals seeking mental health care encounter structural barriers such as cost, limited provider availability, or scheduling challenges. While access can shape which options are realistically available, both TMS therapy and EMDR are generally well tolerated. The type of side effects differs because the treatments work in different ways.
TMS
TMS is a noninvasive brain stimulation treatment delivered in a clinical setting. The most commonly reported side effects are:
- Mild headaches
- Temporary scalp discomfort at the site of stimulation
These effects are typically short-lived and often decrease as treatment continues. Most patients return to normal activities immediately after a session. Unlike medications used to treat major depressive disorder, TMS does not cause systemic side effects such as weight gain, sexual dysfunction, or sedation.
EMDR
EMDR is a structured psychotherapy, so its side effects are emotional rather than physical. During trauma processing, individuals may experience:
- Temporary emotional resurfacing
- Increased distress during or shortly after sessions
- Fatigue following emotionally intensive sessions
These reactions are often part of the therapeutic process as memories are reprocessed, but they can feel intense in the short term.
How They Compare to Medication
Neither TMS nor EMDR involves daily systemic medication. TMS does not circulate through the bloodstream and is not associated with metabolic or hormonal side effects. EMDR does not introduce pharmacologic effects at all. For individuals who have experienced medication-related issues, including weight gain or intolerable systemic side effects, these differences may factor into treatment decisions.
TMS side effects are typically physical and procedural, while EMDR side effects are emotional and processing-based.
What the Treatment Timeline Looks Like
While both TMS therapy and EMDR are structured treatments, their schedules and time commitments differ significantly.
TMS Therapy Schedule
A standard TMS course is typically delivered five days per week over four to six weeks, depending on the protocol and clinical response. Some variations, such as accelerated TMS or shorter protocols, may adjust session timing, but consistency remains important.
Each session usually lasts between 20 and 40 minutes. Because TMS is noninvasive and does not require anesthesia, most patients return to normal activities immediately after treatment.
The intensity of the schedule is front-loaded, meaning appointments are frequent over a shorter period of time.
EMDR Schedule
EMDR is conducted as psychotherapy, typically once per week. Session length often ranges from 45 to 90 minutes, depending on the treatment plan.
The total number of sessions varies based on:
- The complexity of trauma history
- Symptom severity
- Emotional readiness
- Coexisting mental health conditions
Unlike TMS, EMDR treatment may extend over a longer overall timeframe, particularly when addressing multiple traumatic events.
Finding the Right Fit
A structured evaluation focuses on understanding what is driving the symptoms, not simply comparing treatment names. When assessing EMDR TMS options and comparing TMS to trauma-focused therapy, a mental health professional looks beyond labels to identify the underlying pattern of distress.
When comparing TMS and EMDR, providers typically consider:
How Clinicians Choose an Approach
A structured evaluation focuses on understanding what is driving the symptoms, not simply comparing treatment names. When assessing TMS therapy vs EMDR, providers typically consider:
- Primary symptom driver: Clinicians determine what is sustaining the symptoms. Treatment-resistant depression reflects dysregulation in mood-related brain circuits, while trauma-related disorders often involve unresolved past trauma and persistent emotional distress. The underlying driver guides the recommended approach.
- Diagnosis and clinical history: The presence of major depressive disorder, bipolar disorder, or other mental illnesses influences treatment selection. For example, transcranial magnetic stimulation TMS is FDA-approved to treat individuals with major depressive disorder. EMDR, or desensitization and reprocessing EMDR, focuses on trauma recovery and reducing the emotional charge of distressing memories.
- Response to previous treatments: Providers assess how mental health concerns have responded to medication, psychotherapy, or other standard interventions. TMS is often considered when depressive symptoms persist despite several weeks of appropriate care. EMDR may be prioritized when emotional distress is clearly tied to unresolved trauma.
- Immediate treatment priority: Stabilizing mood-related brain activity may point toward transcranial magnetic stimulation TMS, a non-invasive approach that uses magnetic fields to influence neural activity. Processing distressing memories tied to past trauma may point toward EMDR, which follows a structured eight-phase approach to reduce PTSD symptoms and reshape negative beliefs.
- Potential sequencing of care: In some cases, treatments are not mutually exclusive. Providers may recommend stabilizing mood first with TMS before beginning trauma processing, particularly when severe depression interferes with daily functioning. Sequential care can be a valuable tool in complex cases involving multiple mental health disorders.
The decision is not about which treatment is universally better. It is about which approach aligns most closely with the individual’s clinical profile, symptom history, and practical needs. Coordinated support services, such as case management, can also play a role in helping individuals navigate treatment planning, follow-up care, and overall continuity of mental health services.
What Ultimately Matters in Treatment
TMS therapy and EMDR are both evidence-based approaches, but they are designed to address different drivers of distress. One focuses on influencing brain circuits involved in mood regulation. The other centers on processing and integrating unresolved traumatic experiences.
The decision is not about trends or preference. It is about alignment. When treatment matches the underlying cause of symptoms, outcomes tend to be more meaningful and sustainable.
For a structured evaluation and guidance tailored to your clinical history and goals, call 1-855-4CHARAK (1.855.424.2725) or fill out the contact form to connect with the team at Charak Center for Health and Wellness.




